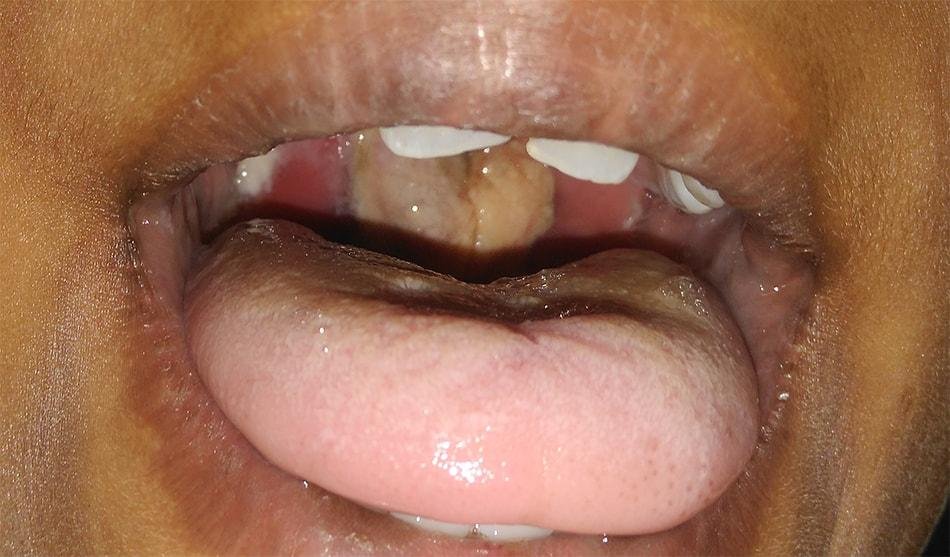
Diphtheria is a life-threatening acute bacterial infectious condition caused by Corynebacterium diphtheriae.
The usual site of infection is the tonsils and oropharynx, but the disease can occur in nasal cavities, larynx or the skin also.
History
The disease was first described in the 5th century BC by Hippocrates and the bacterium was discovered by Edwin Klebs in 1882.
In 1613, Spain experienced an epidemic of diphtheria and the year is known as El Año de los Garrotillos (The Year of Strangulations) in the history of Spain.
Pierre Bretonneau in 1826, named the disease as diphthérite (from Greek diphtheria “leather”) describing the appearance of pseudomembrane in the throat.
Epidemiology
Diphtheria is prevalent in developing countries and mainly affects non-immunized children under the age of ten years. It is almost rare over ten years of age.
Diphtheria is caused by a gram-positive bacteria Corynebacterium diphtheria.
Three different strains of the bacteria are identified, namely gravis, intermedius and mitis. Gravis strain is responsible for the major epidemics of the disease and is associated with higher mortality.
The bacteria lives as a commensal in the human pharynx and produces an exotoxin depending on the presence of a lysogenic bacteriophage (b-phage), which carries a gene encoding for toxin (tox+). The bacteriophage integrates the toxin-encoding genetic elements into the bacteria. Exotoxin has 2 segments, segment A and B. Segment A is the active fragment of the toxin.
The clinical manifestations of the disease are due to the exotoxin produced. Locally the exotoxin causes necrosis of epithelial cells and liberates serous and fibrinous material which forms a characteristic grayish-white pseudo-membrane consisting of necrotic tissue, bacteria, and rich fibrinous exudate. This membrane can cover tissues in the nose, tonsils, larynx, and throat, making it very hard to breathe and swallow.
At later stages, exotoxin principally affects the cardiovascular system, central nervous system, and renal system. Myocardial fibers are degenerated leading to dilated cardiomyopathy and conduction disturbances. Involvement of the nervous system results in polyneuritis. In the renal system, it causes degeneration of tubular cells.
Mode of the spread of infection
The infection spreads by droplets from the upper respiratory tract when infected individual coughs or sneezes and the portal of entry is through the respiratory tract, but rarely via conjunctiva, skin, etc.
It may also be spread by contaminated objects. The incubation period is around 2-5 days.
Some people carry the bacteria without having symptoms, but can still spread the disease to others. Disease progression and carrier status is defined by the host response, virulence, and toxigenicity of the organism.
Clinical presentation
Signs and symptoms may vary from mild to severe. They usually start two to five days after the exposure.
Clinically the child presents with a severe sore throat, dysphagia (painful swallowing), malaise, pyrexia (fever), muffled voice and nasal discharge. The child will look sick, toxic and may have clouded sensorium.
There will be enlarged and tender cervical lymph nodes classically termed as “bull neck appearance”.
Locally, nasal diphtheria presents with unilateral or bilateral serosanguinous discharge from the nose with excoriations of the upper lip.
In faucial diphtheria, there will be redness and swelling over fauces. A dirty greyish pseudomembrane will be seen in the oropharynx associated with green or black necrotic patches, which may spread downwards to affect the larynx. Early removal of the membrane causes bleeding, but it gets easily removed at a later stage. The membrane is highly infectious, and droplet and contact precautions must be followed when examining or caring for infected patients.
In laryngotracheal diphtheria, the membrane over larynx causes paroxysmal exhausting brassy cough and hoarse voice with inspiratory stridor as in croup; hence also termed as “diphtheritic croup”. There will be labored and noisy respiration with a suprasternal and subcostal recession, restlessness, increasing respiratory effort, and eventually respiratory failure. Laryngeal diphtheria rarely occurs without prior pharyngeal infection.
Diphtheria can present at other unusual sites too. These lesions may be found in the conjunctiva, the skin over pre-existing ulcers which may become tender, punched out and with thick edges. The pseudomembrane over ulcer appears as a greyish slough.
At later stages, the child may present with complications. Cardiac involvement causes myocarditis and arrhythmia leading to circulatory collapse. Neurological complications are cranial or peripheral nerve palsies. Renal involvement can cause oliguria.
The differential diagnosis of these patients includes angioedema, epiglottitis, infectious mononucleosis, infective endocarditis, myocarditis, oropharyngeal/esophageal candidiasis, pharyngitis, peritonsillar/retropharyngeal abscess, etc.
Investigations
United States’ Centers for Disease Control and Prevention uses both laboratory and clinical criteria for the diagnosis of diphtheria.
Lab criteria:
- On Albert staining, the bacilli form a characteristic Chinese letter pattern. They are club-shaped with one end border than the other and show a beaded or band like metachromatic granule.
- Microbiological culture: A swab of throat and nasopharynx (or sample of the membrane) should be collected for culture and antibiotic sensitivity. Tellurite or Loeffler media is the specific medium used for culture of diphtheria bacteria.
Clinical criteria:
- Upper respiratory tract illness with a sore throat
- Low-grade fever (above 39 °C /102 °F is rare)
- An adherent, dense, grey pseudomembrane covering the posterior aspect of the pharynx: in severe cases, it can extend to cover the entire tracheobronchial tree.
Other methods
- Schick test: This test is quite obsolete now. The test is performed by injecting intradermal diphtheria toxin.
- Identification of bacilli by the fluorescent antibody technique.
- Elek test detects the development of an immuno-precipitin band on a filter paper impregnated with antitoxin and then is laid over an agar culture of the organism being tested.
Management of Diphtheria
The patient should be admitted and isolated immediately. Obtain throat and pharyngeal swabs from the patient and all close contacts.
Initial treatment starts with a high dose of benzylpenicillin 5 lakh units intramuscular every 6 hours for 6 days. Erythromycin (orally or by injection) for 14 days (40 mg/kg per day with a maximum of 2 g/d) can be given to those patients who are allergic to penicillin.
Diphtheria antitoxin intramuscular (IM) or intravenous (iv, after test dose) should be given as a presumptive treatment while waiting for microbiology confirmation along with antibiotics. This is because antitoxin does not neutralize toxin that is already bound to tissues and delaying its administration is associated with an increase in mortality risk.
- ½ of the dose is given intramuscularly while the other half is given as intravascular
- Laryngeal diphtheria – 48 hours – 20,000 to 40,000IU
- Nasopharyngeal – 40,000 – 60,000IU
- Extensive d/s of 3 or more days, with neck swellings – 80,000 to 1,20,000IU
- Airway compromise should be anticipated and managed by intubation or tracheostomy.
- Cardiac monitoring with or without electrical spacing and bed rest is needed.
- 3 negative cultures 24 hours apart should be obtained to declare the patient as free of the organism.
- Previous infection does not confer immunity; thus, initiation or completion of immunization with diphtheria toxoid is necessary.
- Close contacts and relatives should be treated and immunized. All suspected and confirmed carriers should be treated with erythromycin or penicillin for 14 days.
Complications
Complications mainly happen by 2nd post-op week. The exotoxin can lead to
- Cardiac complications – Mainly cause myocarditis in 2nd week, leads to arrhythmia and possible death. Seen in 60% of unimmunized children.
- Neurological complications – Leading to paralysis of cranial nerves (nasal regurgitation and hypernasal speech due to soft palate paralysis). Extraocular muscles (loss of accommodation, 3rd week) and general polyneuritis (6th week).
- Renal problem – Oliguria and proteinuria.
- Long term – scarring of oropharynx and nasopharynx due to fibrosis and adhesion formation.
The most frequent cause of death is airway obstruction or suffocation following aspiration of the pseudomembrane.
Death occurs in 5% to 10% of those affected.
Prevention of Diphtheria
A diphtheria vaccine is effective for prevention and available in a number of formulations. Three or four doses, given along with tetanus vaccine and pertussis vaccine, are recommended during childhood. Further doses of diphtheria-tetanus vaccine are recommended every ten years. Protection can be verified by measuring the antitoxin level in the blood.
The Global Pertussis Initiative formed in 2001 is the task force working towards global immunizations and disease prevention in infants, adolescents, and adults for diphtheria, pertussis, and tetanus.
The 4 forms of the diphtheria toxoid are as follows.
- DTap is the childhood vaccine and is given at 2 months, 4 months, 6 months, 15-18 months, and 4-6 years. The uppercase D denotes the full strength of tetanus toxoid (7-8 Lf units).
- Tdap is recommended for adolescents aged 11-12 years or in place of one Td booster in older adolescents and adults aged 19 years and older.
- DT does not contain pertussis and is given to children who have had previous adverse reactions to acellular pertussis incorporated vaccine.
- Td is a vaccine for adolescents and adults given as a booster every 10 years or when an exposure has occurred. The lowercase denotes reduced strength diphtheria toxoid (2.0-2.5 Lf units). It is given to those older than 7 years.