Tracheostomy is a common procedure usually performed as part of modern airway management in many specialties like surgical, medical and critical care units. Globally the number of tracheostomies being performed is increasing due to many reasons like cancer of larynx, nasopharynx, severe head injury, spinal cord injury, vocal cord paralysis motor neuron disease etc. Approximately 20% of tracheostomy patients are discharged from hospital with the tracheostomy tube insitu. These patients with permanent tracheostomies need proper long-term care and management.
Inappropriate care can result in unexpected adverse outcomes. Fracture of metallic tracheostomy tube (TT) with aspiration of the fragment into tracheobronchial airway is a rare complication of tracheostomy. In extreme cases, this can fail the whole purpose of tracheostomy by compromising the airway, which necessitates urgent medical attention. Hence there is a need to understand this particular complication, for prevention, early recognition and prompt management.
This is a rare case of a 42-year-old patient, who attended the emergency department with the complaint of mild respiratory distress following aspiration of fractured metallic TT. This report showcases a novel method for the extraction of the same. We also include a review of literature and best practice recommendations for proper tracheostomy care.
Case report
A 42-year-old male patient presented to emergency department with complaint of mild respiratory distress following aspiration of a broken tracheostomy tube. This happened while his wife was attempting the removal of tube for routine cleaning. She noticed that the tube part was missing and only neck plate (shield) was in place. The patient has undergone tracheostomy 3 years back due to bilateral abductor palsy following total thyroidectomy for papillary carcinoma thyroid in another institute. For last 2 years, he never had follow-up with the hospital where he was initially treated and continued to use the metallic tube for two years.
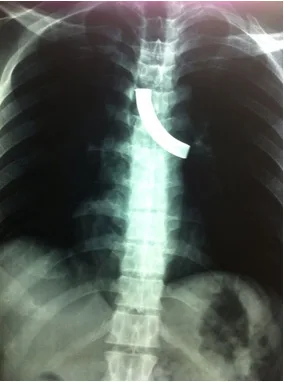
At time of presentation in emergency room (ER) the patient was hemodynamically stable with mild tachypnea (respiratory rate was 22/minute). His oxygen saturation was 97% on air. Neck examination revealed a patent stoma. On auscultation air entry was reduced on left side of chest. Rhonchi were present. A chest X-ray (postero-anterior view) revealed fractured TT in left main bronchus. He was given oxygen inhalation, nebulization and steroids in the ER and then shifted to operating room (OR).
In the OR, intravenous sedation was given. Patient was pre-oxygenated through the stoma. Under apnea-oxygenation-apnea technique a 0° 4mm Storz® nasal endoscope connected to camera and monitor was passed through the stoma with minimal difficulty, with neck extended. The broken fragment was visualized in lower trachea and left main bronchus. The fragment was gently dislodged with bronchoscope forceps and then withdrawn slowly along with the endoscope. The patient was oxygenated again to maintain the saturation. The scope passed again to visualize the tracheal lumen. The tracheal mucosa was appearing to be congested and edematous. After removal of the broken fragment, a new PVC tube (8 mm) was inserted and secured into the tracheostomy site. Inspection of the fractured piece showed severe corrosion at junction between tube and neck plate.
The patient was observed for 12 hours in the intensive care unit (ICU) and was then shifted to ward. The postoperative period was uneventful. He was discharged on next day with instructions for regular follow up and was educated regarding tracheostomy care.